Osteochondrosis forces the body to keep the lower back muscles tensed, which reduces the load on the spine. Patients seek a more comfortable position and try not to alter it to reduce discomfort.
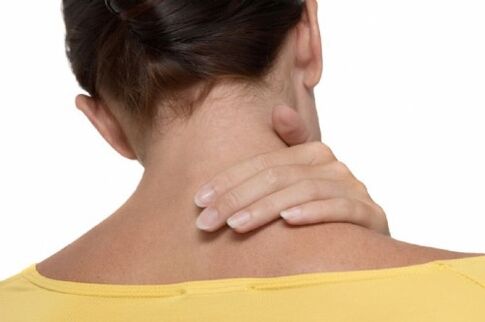
The main steps
The disease is progressive, so there are corresponding symptoms at different stages, and the diagnosis helps the doctor to prescribe the correct treatment plan. Symptoms of lumbar osteochondrosis:
- In the first stage, there is obvious discomfort and insignificant pain in the lumbar spine;
- The second stage is accompanied by destruction of the annulus fibrosus, which leads to fusion of the vertebrae with each other;
- Subsequent formation of intervertebral hernias and marked deformation of the spine, accompanied by severe pain;
- The fourth stage of lumbar osteochondrosis results in complete disability of the patient: the destruction becomes more severe, preceded by severe pain and difficulty with movement.
At any stage, the development and further treatment of osteochondrosis depends on the localization of the disease to a specific part of the lower back. The therapy is aimed at reducing pain, eliminating inflammation, normalizing metabolic processes in the cartilage tissue of the intervertebral disc.
Lumbar osteochondrosis is a dangerous degenerative disease of the spine that causes a degenerative process. It is located in the corresponding area, which is characterized by chondral ossification or destruction of the intervertebral disc. More than 80% of the course of the disease is accompanied by pain radiating to the legs. Painful symptoms are caused by overgrown tissue squeezing the spinal nerve roots, medically known as lumbar sciatica.
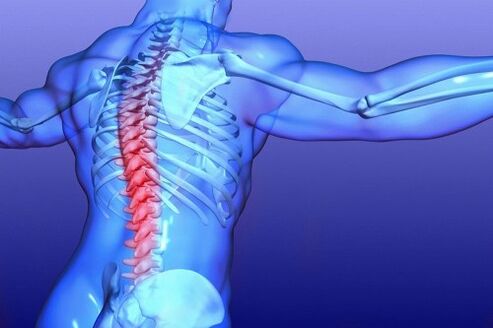
signs of initial stages
Symptoms of lumbar osteochondrosis are accompanied by a dull pain that usually goes unnoticed. Unpleasant sensations in the back or hips after moving heavy objects and sudden movements. The initial degenerative process begins in the intervertebral lumbar region.
There is no specific change in the function of the spine, but the morphological process of inundation of cartilaginous tissue continues, accompanied by the following signs:
- uncinate increase;
- Minimal disc displacement with fibrocapsular rupture.
Clinical Signs - Severe pain after physical exertion and prolonged (often) sitting in an uncomfortable position.
Sometimes the first stage is called the preclinical stage because lumbar osteochondrosis may not actually manifest itself.
second stage
Symptoms at this stage are chronic pain that radiates to the pelvic organs, buttocks or legs. Both relapses and remissions are characteristic. Basically, deterioration is observed after physical exertion.
The third stage
A gradual process leads to the formation of a hernia and all the consequences that follow:
- Neurologic symptoms (dizziness, headache, fainting, tinnitus, and loss of consciousness);
- kidney and genitourinary problems (uncontrollable urination);
- Problems with the cardiovascular system (arrhythmia).
In the third stage, in addition to medication and physical therapy, treatment may include surgery to avoid spinal cord compression and unnecessary complications.
fourth stage
The final stage is accompanied by calcification of the damaged intervertebral disc. The pain has subsided a lot, but the deformation of the spine continues. The body activates defense mechanisms, starts the ossification process, leads to a decrease in the epidural space, increased compression of the spinal cord, and disrupts the work of all systems controlled by it. In simple terms, cartilage turns into bone and grows. From here, the many dangerous symptoms that characterize the third stage appear, but in a more severe form.
Long-term complex therapeutic and surgical interventions are required.
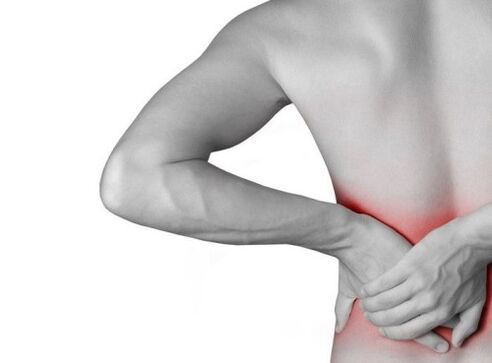
How to distinguish where the lesion is located
Crush of certain nerve endings and segments has its own osteochondrosis signs and symptoms:
- Damage to the L1, L2 roots of the spine - Severe pain, numbness in the groin area and inner thigh. Progression of osteochondrosis of the lower back with hernia, characterized by lumbar ischialgia in both lower extremities;
- When limited to the lumbar L5, shooting pain is characteristic of thumb irradiation with reduced sensitivity;
- Numbness with severe pain in outer thigh to calf, problem is compression of nerve root S1.
Treatment follows diagnosis by MRI.
Symptoms of lumbosacral osteochondrosis
The localization of a disease has a direct impact on its course and symptoms. Degeneration of the lumbar spine can lead to myeloid claudication. The lower spinal cord receives a limited blood supply, which can cause leg weakness and frequent urination when walking. After proper rest, the symptoms disappeared.
Ischemia of cauda equina neurons is the main cause of intermittent claudication:
- anemia in the area around the legs;
- tingling and tingling sensation when walking;
- Symptoms that rise from the legs to the groin area of the genitals over time;
- Leg strength recovers after rest.
Lifting heavy objects in the presence of lumbar osteochondrosis can cause compression of the Adamkevich arteries and complicate the course of spinal disease. There is paralysis - from mild to severe, waste incontinence, atrophy of muscle tissue, formation of bedsores.
What Causes the Development of Osteochondrosis
In most cases, the development of osteochondrosis is thought to develop gradually due to bipedal walking, but other predisposing factors play an important role in the development of spinal disorders, including: lack of exercise, impaired metabolic processes, body weightOverweight, weightlifting.
A complex interplay of adverse factors, the formation of a prolapse (herniated disc) leads to narrowing of the epidural space and compression of the nerve roots.
medical method of treating disease
Staged treatment of lumbar osteochondrosis is carried out after accurate diagnosis of the patient's location, stage and individual characteristics. The main methods are physical therapy, reflexology, drug support aimed at reducing pain and stopping inflammation, herbal remedies. Surgical intervention is required if treatment is ineffective or not possible without surgery due to neglected disease.



















